
Melanoma Success Story: Joan (age 45)
- Read our in-depth interview with Joan about her journey with melanoma
- Read more success stories about patients like you
- Get the CTOAM brochure
- Download the free CTOAM Precision Oncology ebook
Get a Precision Second Opinion now!

Patient Presentation: Stage IV Metastatic Melanoma
Joan is a 45-year-old woman with stage IV metastatic melanoma. At the time of her diagnosis, there was a new targeted trial with a drug that targeted a key mutation called BRAF V600E. Joan’s oncologist ordered the standard immunohistochemical (IHC) testing of her biopsy sample. From the results, the oncologist determined that Joan’s tumours were BRAF mutation negative. And therefore, she would not be a candidate for anti-BRAF therapies.
Joan was given the option of standard dacarbazine chemotherapy, which has been reported to provide a 2.5 month progression-free rate and a 10.7-month median overall survival advantage. Since her disease would not respond to standard treatments, her oncologist told her that they had no other treatment options for her.
She was told to get her affairs in order. Joan wasn’t ready to accept this – so she reached out to CTOAM.
Melanoma Success Story
How CTOAM Helped Joan
1. Introduced Advanced Diagnostics
First, we
recommended that Joan get a PET/CT prior to any treatment, in order to establish the exact extent of
her disease. Our cancer research and patient advocacy experts suggested a local private clinic based in British Columbia (Premier Diagnostic Center). This local company is our
first choice for PET/CT scans because it offers:
- Very fast results
- Low cost compared to other clinics
- Excellent radiologists
The radiologists at Premier Diagnostic Center report the SUVs (Serum Uptake Value) of every tumour – unlike many other clinics we have dealt with. Please note that CTOAM has no financial affiliation with Premier Diagnostic Center: our only goal in recommending them is to offer patients the most benefit.
How to Detect Melanoma
What is a PET/CT Scan?
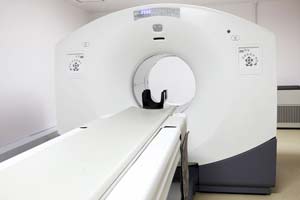
PET/CT, unlike other forms of medical imaging, is able to identify active tumours at a very small size, based on the biological activity of the tumour.
While most forms of imaging look at the density of the tumour and compare it to the Cancer Care Research and Advocacy Specialisttissues, PET/CT uses a harmless radioactive isotope that is bound to a sugar molecule.
Since tumour cells are constantly growing and therefore highly metabolic, they drink up more of the sugar-isotope solution than the surrounding tissues, and any tumour will glow like a Christmas tree light.
Since only live tumours will drink the sugar-isotope solution, PET/CT can tell if a tumour is alive or if it has been affected (killed) by a specific treatment. No other form of imaging can reveal this essential information!
Furthermore, since the amount of the sugar-isotope solution a specific tumour drinks depends on how fast it is growing, a PET/CT can determine how aggressive a specific tumour is compared with other tumours in the body. This can allow doctors to focus on the tumours that are most likely to metastasize.
Joan’s PET/CT revealed numerous metastatic sites. It also provided us with a baseline SUV reading for each tumour. This allows us to use future PET/CTs to confirm if her tumours are responding to treatment or not.
Next, CTOAM obtained a sample of Joan’s tumour tissue and sent it for tumour DNA sequencing. We looked for cancer-causing mutations in the DNA of over 340 genes involved in melanomas and other cancers.
Medical Advancements: At that time, the tumour DNA sequencing panel was not nearly as advanced as it is now. This meant the turn-around time for this assay was over three months (compared to today, between 4-6 weeks).

3. Clinical Trial Research and Support
In order to provide Joan with an interim treatment solution, our experts researched the latest peer reviewed data and oncology conferences for advances in treatment of metastatic melanomas.
Interestingly, CTOAM’s research revealed some very significant data on new drugs that target two arms of the immune system, known as CTLA4 and PD-1.
Metastatic Melanoma Treatment Options
What is CTLA4?
CTLA4: The cytotoxic T-lymphocyte-associated protein 4 (CTLA4) is a receptor that functions to downregulate immune responses so that the immune system does not attack and target healthy cells.
How T-cells work: The immune system sends T-cells to investigate a foreign object or tumour. The T-cells surround the foreign object / tumour and create an immune response that causes the activation of different arms of the immune system.
Activating the immune system: The immune cells do this by releasing a multitude of growth factors and resources required for a rapid expansion of the immune system and a proper immune response. However, these growth factors and resources can also be hijacked by the tumours, allowing them to grow rapidly and metastasize.
How CTLA4 affects melanoma: In some cancers, such as melanomas, the tumours produce a high amount of the CTLA4 protein, causing the tumours to be protected and hidden from the immune system. This is one of three known mechanisms that tumours use to avoid detection by the immune system. The other two are known as the PD-1 axis and IDO axis.
Our cancer specialists reached out to a local oncologist who’d been instrumental in recently bringing a new CTLA4 inhibitor to British Columbia. The drug was called ipilimumab. Unfortunately, this oncologist was not having a lot of luck with ipilimumab. So we researched the latest clinical data regarding administration of this new drug.
CTOAM’s research revealed important new data showing that:
- The current dosage of 3mg/kg was ineffective.
- Combining a steroid called budesonide and another medication called GM-CSF could provide significantly improved results in patients. (GM-CSF was commonly used to stimulate the production of white blood cells in patients with neutropenia – i.e. low neutrophils – that were undergoing chemotherapy.)
For the interim treatment, we recommended the 10mg/kg dose of ipilimumab (standard was 3mg), combined with budesonide and GM-CSF.
Our team also suggested that Joan’s oncologists look into obtaining future access to the newer (and yet-to-be-named) drug that targeted the PD-1 axis, since the pre-clinical data was very impressive.
Happily, many of Joan’s tumours responded very quickly to this unique combination of drugs.

4. Genetic Testing During Treatment
During the course of her therapy, the tumour DNA sequencing results of her biopsy identified a BRAF V600E mutation. This had been missed by her initial pathologist at BCCA.
This important discovery created two new treatment opportunities for Joan:
- New targeted therapy: A new drug that targeted BRAF V600E mutations called vemurafenib was providing significant benefits to patients with BRAF-mutated melanomas, and had recently been approved by the FDA.
- Liquid biopsy for treatment monitoring: Since a mutated gene is unlikely to get fixed during the course of disease, and since we now knew that ALL of Joan’s tumours carried the BRAF V600E mutation, we could use a blood based liquid biopsy test to assess the level of BRAF V600E mutations in her blood, in order to determine how she was responding to the drug.
Treatment Monitoring for Melanoma
What are Liquid Biopsies?
Liquid biopsies detect circulating tumour DNA (ctDNA), and measure the ratio of the mutated (BRAF) to the non-mutated (BRAF) genes, in order to provide us with a rough idea of the actual amount of cancer cells in a body at a given time.
More accurate treatment monitoring: Testing all of the body’s tumours at the same time using liquid biopsies is much more accurate way of determining responses to immune checkpoint inhibitors such as CTLA4 than other methods, such as radiographic imaging and other non-specific blood-based tumour markers such as CEA, and CD19-9/ 15-3, which are used by the public medical system.
This is because different tumours interact with the immune system at different stages of the disease. Looking at a complete body-wide, drug-induced, anti-tumour response is essential for determining how well the treatment is working.
Importantly, patients are not subjected to ionizing radiation (like with CT and PET/CT scans).

Using Liquid Biopsies and PET/CT to Determine an Immune Response
A mid-treatment PET/CT showed mixed results with the majority of Joan’s tumours showing significantly lower SUV levels (this indicates tumours that they are dying and responding to the drug), with some of her tumours having already shrunk.
- Public system shortcomings: However, her doctors were alarmed at what appeared to be some new growths, based on very low, non-specific SUV levels in certain parts of her body. Based on the RECIST response criteria, this finding would indicate what is known as a “mixed response,” and that the drug is not working as well as we had hoped for.
- Advancements in cancer research: CTOAM explained to her treatment team that this “mixed response” was based on the mechanics of the drug, and is referred to as pseudo-progression. Since ipilimumab removes the excess CTLA4 cloak surrounding tumours, the immune T-cells start to recognize them as actual tumours and infiltrate the tumour cells in order to break them down.
How Ipilimumab Works
This infiltration of the immune cells into the actual tumour results in a tumour that is much larger than it was previously was. And since there is activity inside of it from the T-cells attacking the tumours (immune response), it would show some very low SUV levels from a PET/CT scan.
In other words, there were likely many small microscopic tumours throughout Betty’s body that were too small to be detected previously via PET/CT, but which could now be seen because of the immune cells entering the tumours, making them large enough to be detected.
In order to determine if the mixed response was due to immune infiltrates rather than disease progression, we performed a ctDNA assay, which showed no presence of the BRAF V600E mutation, indicating pseudo-progression as the cause of the mixed PET/CT results in the majority of her tumours.
5. Clinical Trial Support and Advocacy
The field of precision oncology is constantly evolving: innovative discoveries and new targeted therapies emerge each day.
Just as Joan was ending her ipilimumab treatments, her community oncologist – the one instrumental in bringing ipilimumab to British Columbia – was able to provide her with access to a new PD-1R inhibitor called pembrolizumab, via clinical trial by distance.
However, only patients who did not have a BRAF V600E mutation were allowed access to this trial. This is because, if they had this mutation, they could be treated with vemurafenib.
This presented CTOAM with a dilemma. We could either:
a) Share our newfound knowledge of Joan’s BRAF mutation with her treatment team and the medical system, which would result in her not being able to enter the pembrolizumab trial; or
b) Withhold this information so she’d be able to enter the trial.
Once again, we hit the books and did an extensive review on both vemurafenib and pembrolizumab. Our researchers uncovered newly published trial data showing pembrolizumab was vastly superior to any known treatment of melanomas, and had minimal side effects.
Furthermore, melanoma patients who took both ipilimumab and pembrolizumab had some of the most drastic responses ever to be recorded in the history of melanoma treatment.
Due to the overwhelming evidence that the clinical trial would greatly benefit Joan, our choice was clear: we suggested that Joan enter the pembrolizumab trial and only release the BRAF mutation data to her treatment team if the pembrolizumab was not effective. In that case, she could then go onto vemurafenib.
After further research and consultation with her oncologist, Joan was provided with experimental access to the PD-1R inhibitor pembrolizumab.
6. Patient Outcome
New data is showing exceptionally long-term survival rates for many melanoma patients that have taken both ipilimumab and pembrolizumab. And Joan’s recent PET/CT failed to find any evidence of her disease.
Currently, Joan remains cancer-free – well over two years after first starting her treatments via CTOAM.
Perhaps just as significant, we feel very positive about Joan’s options should her disease recur. If that happens, we can try anti-BRAF therapy, as well as the next generation PD-1 ligand inhibitors. The latter are showing improved benefits to that of the first generation PD-1 receptor inhibitors, such as pembrolizumab.
Conclusions
As you can see, CTOAM’s advanced diagnostics, records review, and consultations can result in significant benefits to a patient’s outcome. Having access to a team of precision oncology specialists, doctors, and patient advocates can make all the difference in the outcome of your disease.
If you or a loved one has cancer, contact us today so we can do a brief review of your medical records. CTOAM’s cancer research and patient advocacy experts will ensure that you have access to the most advanced tests and treatments available for your unique form of cancer – as close to home as possible.
Get a Precision Second Opinion now!
Changing the face of cancer care, one person at a time.