
Melanoma Success Story
Interview with Joan, CTOAM Patient
- Read more about Joan’s success story
- See all patient success stories
- Get a Precision Second Opinion now!
"Alex was just so positive – we enjoyed our phone calls with him because we talked to him, we were always like, 'okay, we can do this!' There was always hope after we talked to him. There was always something we could be doing more of. You know, drink your green tea, take all your nutraceuticals…there was just always, always something positive." – Joan
Joan’s Story: An Overview
Read the summary below to learn about Joan’s story with melanoma. You can also see her case study to learn more about the precision oncology methods that CTOAM used to help her.

Joan had had a mole on her underarm for years. She’d gotten it checked out numerous times by her GP, just to be safe. It never rang any alarms for the GP who kept saying, "it looks fine".
Then it started to bug Joan a bit, rubbing up against her t-shirt. She went back to her GP again to get it checked, just to make sure. "It looks fine" was again her GP’s verdict.
But then it started to open up a bit and change more. Joan had it removed and discovered it was melanoma. She had the surrounding lymph nodes removed as well. At that point it was assessed by her oncologist as being around stage 2 or stage 3. Joan and her husband figured the worst was over – that the surgery had solved the problem.
Soon after, though, they learned the cancer had quickly escalated to stage 4. They asked to change oncologists because their first oncologist hadn’t been the right fit for them. Their GP recommended a new one who was a better matched for them. Around that same time, Joan and her husband also decided to hire CTOAM to ensure they would have the best chance possible at beating the odds.
While all this was going on, Joan had genetic testing done through the BC Cancer Agency. This was done to see if she was BRAF positive and therefore eligible for a certain clinical trial her oncologist suggested for her. The test results came back negative, so Joan didn’t join the trial.
She then had her genetic testing done again, this time more comprehensively, through CTOAM. With Alex’s in-depth analysis, we learned that Joan was, in fact, BRAF positive. In hindsight, it’s a good thing that Joan didn’t join the clinical trial, since those drugs would have only worked for a few months – and CTOAM had, in the meantime, found a much better drug combination that would cure her permanently!
Alex recommended a few different drugs for Joan. One of them was a standard drug, but at a signficantly higher dosage than the standard dosage (10mg vs 3mg). Joan was able to access to all the drugs recommended for her through the data that CTOAM provided. Even better, all of her drugs ended up being fully covered by her husband’s insurance. This is because Joan was able to provide the insurance company with the studies and data (provided by CTOAM) to back up the request. That’s $250,000 worth of treatment – not available through standard care – completely covered.
In addition, with CTOAM’s help, Joan was quickly accepted into a clinical trial for immunotherapy. Within a few months of starting the treatment, a liquid biopsy test (arranged by CTOAM) showed that Joan was already cancer free! She continued that treatment, entirely free of charge, for about a year in total. Joan has remained cancer free ever since!
Interview with Joan
Read this long-form interview with melanoma survivor, Joan, to hear her full story about finding CTOAM and how she went from stage IV melanoma to being 100% cancer-free.
Tell us a bit about you and how you found CTOAM.
I’m married, with two kids, and my husband, Raymond, was very supportive in all this. When it all started (when I got the diagnosis), my husband started to research on the internet and he said to me: "don’t even go there – don’t look on the internet." Because there was so much information to look through and he didn’t want me to [be overwhelmed].
So I didn’t touch the internet pretty much the whole time that I had cancer.
There was only one time when Raymond said, "okay, here is something that you can look at", and it was the medication that I ended up taking. He said to me, "these are the only good statistics that I’ve found for melanoma: this is what will give us hope. So you can read this article." Other than that, he just spent hours researching on the internet. And he’s good at that – at collating all the information.
So my husband’s the one who found Alex, just through his internet search. And he started the initial contact with Alex as well, and vetted it before bringing me into it. He wanted to make sure that it [CTOAM] was good and something that we were going to go ahead with.
That’s really great that you managed to avoid wading through the internet.
The reality is that there are no good statistics for melanoma. Because all the medication that’s been [successful for melanoma patients] is all new. For example, I’m now only a few years past [taking the drug] and other people are maybe five or ten years past. So there are no long term studies that are really positive for melanoma. So the internet is generally not too good for melanoma!
How did you first find out about your diagnosis?
It was just a mole on my underarm – not even a sun-exposed part. Like, for all the lifeguarding and time I’ve spent out in the sun in my teenage years...this one was in my armpit, just a mole.
I’d actually already seen my GP about it. Typical story: she said, "yeah, it looks fine". It had been there for years, but it was in a spot where my t-shirt started to rub it and it was starting to bug me a little bit. But she said it looked fine.
And then it started to really change. It opened up a little bit, which is when I went a got it removed and found out that it was melanoma.
It was first diagnosed as just this stage I, stage II cancer. And then they found it in my lymph nodes. And then they found it in my lungs. It was a few months [until I got the stage IV diagnosis]: I was diagnosed in September and it wasn’t until March of the next year that they told me I had stage IV.

And during those months in between, did your oncologist or doctor do anything?
Well, it was a bit of a mess. They removed the mole and then they checked the lymph nodes. Our oncologist at the time – I think he’s brilliant – but his communication skills were not great. We needed information and couldn’t seem to get it from him. He went away on vacation and the surgeon said to us, "you need your lymph nodes out". But our oncologist had been saying, "no, I don’t think she needs them out".
And I’m like, "if there’s cancer in me, it’s coming out!" So they did take all my lymph nodes out.
In hindsight, I bet that the oncologist thought that the spots in my lungs were cancerous, so he was probably already thinking stage IV and not telling us. And that I didn’t actually probably need to get my lymph nodes out, because the cancer had already spread.
(They had seen little spots on my lungs on the scan. But, at the time, I was 42; anyone that age is going to have spots. I still have spots on my liver that nothing’s happened to – they’re not cancerous – they’re just there because now I’m 45. So the oncologist said, "everyone has stuff like that".)
And yeah, he didn’t diagnose it right away. He waited until the tumours grew and then gave me the stage IV cancer diagnosis. And then we fired him.
He just wasn’t a good fit for us. We needed more information and we needed a bit more conversation. When he gave us the stage IV diagnosis, he brought a student in there with him to come and watch. I don’t know why...maybe to watch us react to a stage IV diagnosis? I mean, I understand they have to learn, but...yeah. There just was a bit of a personality disconnect, I think.
So we just went to our GP and said, "this is not working". She gave me a referral to a new oncologist.
Why did your GP miss your original diagnosis? Where did she go wrong?
Honestly, I think she’s beating herself up about it. The first few times I went back to her, we’d honestly be in tears together, and she’d pull out her text book and say, "was it anything like this? Was it anything like that?" She really was trying to understand how she missed it. I mean, the reality is that she looked at the mole at the time and it didn’t look like cancer to her in any way. And so that was the end of that, until it got worse.
So my GP had her pieces that she helped with – she helped me out with getting the new oncologist and with getting the mole removed. You know, there’s just little things that she could do here and there, but she’s just a little fish in this big picture. So I dont know there’s much more she could do, honestly. I mean, if you miss that diagnosis, but...you know, she’s a GP – how are they an expert in everything? They’re not, right? So there’s no blame on her, at all. It is what it is.
What we’ve learned through all of this is that everyone – each doctor – has their limits and the only person who’s going to bring it all together is you. The only one who’s going to spearhead and drive you getting better is you.
And that was one of the great things about CTOAM: Alex really brought together a lot of the different parts that we’d already researched a bit. And he put a lot more science behind it and behind why.
We have Inspire Health here in British Columbia. They do natural diet, exercise, meditation, and yoga – all the extra stuff for cancer. So I had already gone to them and done a lot of the diet changes.
But then Alex was able to provide science to back up a lot of [those changes] and also gave me ways to augment them.
He also recommended more [diet changes] for me, and this time there was science behind it [and it was more personalized]. It gave me a bit more belief in it, knowing that it had been researched: it wasn’t just airy fairy; there was some science behind it.
For example, Inspire Health had recommended some exercise, but Alex told me to focus on the strength training, since it’s going to draw the blood away from those tumours and straight to your muscles. And I’m like, "okay! I’m going to the gym!"
I’ve never eaten better, never done more exercise in my life! So Alex brought that together more, as well as the treatment side of it.

What happened between having the initial stage 1 diagnosis to stage IV?
So my husband, since he’d been researching drug options [from the latest study results], knew the best meds that I should be on from the start. When it was diagnosed as stage IV, that’s when things went into high gear.
Before we got the stage IV diagnosis, we had kind of thought that it was treated. When it was at a stage III, it was in my lymph nodes and then they were removed – so we kind of thought that it was taken care of at that point. Interestingly, the doctors were still looking into a clinical study that you were accepted into if you were BRAF positive.
I kind of fit the stereotype that I would’ve been BRAF positive. So the cancer clinic took my tumour and had it genetically tested. They didn’t find the BRAF genetic mutation. So, in the end, I wasn’t accepted into the trial.
But when we actually had it done properly through CTOAM – and Alex [analyzed the results] more thoroughly – it turns out that I was BRAF positive!
And, in hindsight, it was good because the medication they were going to give me would’ve only helped for 3 or 4 months – it wouldn’t have been the total cure that the immunotherapy was. So it was actually good that they had a crappy genetic testing process at the cancer clinic! It doesn’t bode well for other people, though. Especially considering that BRAF is a very common marker, and they were looking specifically for it – and still manage to miss it...
And after you were given the stage IV diagnosis, what happened?
So at that point, we hired CTOAM and we also had a new oncologist. There were a few different drugs that Alex had recommended. One of them was a standard drug. For that standard drug, 3mg was the standard dosage recommended by the cancer clinic. But according to Alex’s research, he said that I needed to have 10mg dosage. He said the studies were showing that the 10mg dosage is far and away better than the 3mg dosage: "If you’re going to do this, do the 10mg."
My new oncologist wouldn’t agree to it because it was outside of her protocol. She was very clear in saying, "I’m not comfortable going outside of the protocol with you".
So Alex suggested the North Vancouver oncologist, Dr. Klimo.
And my oncologist said, "I’m more than happy to give you a referral to Dr. Klimo and to be a continued part of your treatment process while you go and do that. So she referred me over to Dr. Klimo, and we saw him, and he got us into the North Vancouver cancer agency with one of his associates who still can admit there. And I got the 10mg dosage through there. So we paid for the additional 7mg and the cancer agency still paid for the 3mg portion.
There were four treatments at $50,000 a treatment. So we started fundraising, thinking, "okay, how are we going to do this?" And the answer is that you fundraise, you remortgage your house, you figure it out. We had a house and we had friends. We’re not super wealthy, but we could survive and come up with that money somehow.
But! There was an amazing nurse at the cancer agency in North Van. Her job is basically to get funding for patients. So she wrote letters to my husband’s insurance company. I’m a private contractor, so I have no coverage. But my husband had coverage through Blue Cross. She wrote letters to them that said, "look at the studies..." and she sent them studies of what the success rates were for 3mg compared to 10mg. And the insurance company approved it!
They paid for my treatment. It came out to, like, $250,000 in the end and they paid for it. So, yeah, that was pretty amazing.
So I got that 10mg treatment. And then, immediately following that, immunotherapy was coming out basically as a stage IV trial to teach clinicians how to administer the drug. So I got in on that immediately following the 10mg treatment, which is what the research said was best to do. And that was that.

And what happened when you got into that clinical trial? Did you have to go anywhere?
No. I think that because it was a stage IV trial, there was a lot less required. I still went over to north van every three weeks for the first part of it, because it was IV (intravenous). I think I started in August 2014. I didn’t have to do anything; I didn’t have to answer any questions, I just went there for my treatment.
Basically, I had permission to do it for as long as I could tolerate it. So we knew that it was working by October. I had a blood test [liquid biopsy] done, recommended by Alex where they can tell whether cancer is there in the bloodstream. And it was totally clear – there was nothing in it. Alex actually had it re-tested because he’s like, "I actually wasn’t expecting that!" So he had it re-tested and, again, there was no sign of cancer in my body at that point already, in October.
But I continued with the treatment anyways for as long as I could tolerate it. It ended up being about 23 or 24 treatments – pretty much a full year.
And that was entirely free for you?
Yeah, totally free.
What process did you go through to get the PET/CT scans done?
I don’t fit into the protocol of getting a PET/CT scan done through the BC Cancer Agency. But of course it’s recommended, so I wanted to get one. When I needed to get one, there was only one in BC at the time – and it happened to be down. So I had to go to Seattle for it. And we had to figure out how to do that. But Alex recommended someone – a medical travel agent – and she hooked us up with everything. So they did all the arrangements, everything.
After we had that one done in Seattle, my oncologist at the cancer agency started sending us for them here. So they were paid for by BCCA then. I think she realized that we were going to do it anyway, she might as well make it a bit easier. There are certain protocols, I think, that are easier to bend than others, and I think this was one of them. So the Seattle one was the only PET/CT we had to pay for and then she sent me for two more. When it came back as all clear, she then recommended switching to a CT scan for ongoing monitoring. So I’ve been doing CTs for ongoing monitoring, one every 6 months.
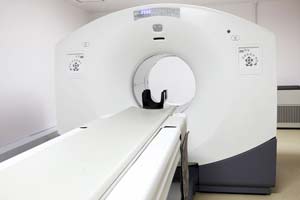
Are you still doing the CT scans now?
For my next CT scan, I’ll be at the three year mark of all clear, so my oncologist is talking about changing to one scan per year (instead of every half year). She’s suggested doing one scan per year for the next 10 years. You don’t really want to be scanned too much, but you also don’t want to miss something.
You know, it’s interesting being on the other side of it now – going from being monitored and scanned so frequently to now so infrequently. It’s anxiety provoking, actually, to change to [being scanned only once a year] because a lot can grow in a year. Not much can grow in six months. You might get a bit anxious or whatever, but you also think, “eh, it’s only been six months, nothing’s happened, right?” But in a year, I don’t know...it feels like something could’ve happened in a year.
But my oncologist is cautious. So I kind of have to put my faith into her. She’s smart and very cautious, so I need to get my own psyche around doing it once a year now. It’s more of an emotional psychological thing.
How was your experience with CTOAM?
We have only good things to say about CTOAM.
Alex was just so positive and we enjoyed our phone calls with him because after we talked to him, we were like, "okay we can do this!"
There was always hope after we talked to him – there was always something we could be doing more of. Like, I still drink my pot of green tea every morning. You know, drink your tea, take all your nutraceuticals...there was just always, always something positive.
And it was nice that [we didn’t need to go to an office to see him]. We had so many appointments at that point, it was nice to just sit in the comfort of our house and talk to him. He did a powerpoint presentation with us and he really educated us well. So I felt like I had a bit better of a grasp of what was going on.
You know, he just felt really smart to me! He would explain it and then he’d dumb it down and then he’d dumb it down another level and I’m like, "yeah, still don’t get it" and he’s like "okay! Imagine you’re an employee and you’re going into a building and you have a badge to get in…" And I’m like, okay! Now you’re talking! I’m following you now! And I have a medical science background even!
So I felt really well educated and I felt empowered by knowing the science behind it.
And if we needed to talk to him, he was always there. There was only hope and positive things when we talked to him.
And Raymond had also done a lot of research in the background and felt that Alex was recommending the same sort of things that he’d found in his own research around the medications and things like that. So we didn’t feel like anything was off the wall.
And it was interesting because my dermatologist had said to us, "you need to be the squeaky wheel. If you’re gonna get anything, you need to be the squeaky wheel." And we were like, "well what do we squeak about? We’re happy to squeak but we don’t know what to squeak about!"
And Alex was the one who directed us, saying "this is what you need to do, this is what you need to get". He also figured out how to get what we needed to get. And so learned how to be the squeaky wheel. Because otherwise, how do you know what to do? How do you know you need 10mg of a certain drug instead of 3mg? I wouldn’t have known how to get that treatment. I wouldn’t have known how to get the Klimo referral or even that I needed that treatment in the first place.

When you were deciding to hire CTOAM, did you have any hesitations about what your oncologist would say? Or fear that you would offend them?
No. I feel like you need to be the expert of your own body. There’s no way that an oncologist, with a caseload that they have to manage, can be the expert in every up and coming medication, type of cancer, and so on.
And if I had an oncologist who thought they were [an expert in every aspect of cancer care], I wouldn’t trust them.
You know, we didn’t come across any issues at all. Our oncologist supported us to do what we felt we needed to do.
However, we also didn’t disclose everything that we had done [outside the public system] to our oncologist. Like, when we had the genetic testing done and I knew that I was BRAF positive, we didn’t tell her a lot of those results because we wanted to be in control of the path that we were going down. We didn’t want her to have any information that would then [obligate] her to tell us, “well this is the protocol now” and lead us down a different, [less effective] path.
So there was some information that we kept to ourselves.
But overall, she was fine with it. And that’s why we switched from our original oncologist to her. We were happy with her because of her personality – we could speak to her and tell her our thoughts. We were up front, saying, "we’re researching other stuff and we’re looking at alternative therapies."
And, the thing is, you can’t dispute the science!
Like, when you say, "the research says that we should have 10mg", that’s a fact. And she didn’t disagree with that; she just felt bound by the protocols. And it didn’t go against her expertise – she agrees that the 10mg is a better treatment. She just can’t give it to us.
I think that as long as you’re not trying to undermine your oncologist’s knowledge – and instead you’re augmenting it, and showing them the studies – I feel like they need to be open to that kind of thing. Especially in the field of oncology, where everything is changing so much all the time. And in our experience, they were open to it.
What would you say to someone whose oncologist is not open to other treatment options?
That’s when I would leave that oncologist. If you’re not going to work with me, then you’re not the right person to treat me!
Did you have any hesitations about hiring CTOAM and paying for it out of pocket?
We didn’t have any hesitations about it. We really felt that we needed help to figure out how to be the squeaky wheel.
And [it was also because] my husband had already found these new medications [through his own research] and knew that this was where our hope was. We knew that the old medications [weren’t the answer] and that we needed to get this new medication.
So we already knew that we weren’t going to be able to follow the protocols of the BC Cancer Agency.
And maybe because I work in the private field – I’m an occupational therapist, so a lot of my clients are WorkSafe clients or they’re ICBC clients. So they’re already involved in the medical system; they already know that there’s more than one tier to our medical system. You don’t walk in and automatically get the best treatment. That’s not actually the way our medical system works, unfortunately. They give good treatment and a lot of times it’s fully adequate. We go into the emergency all the time with our kids and see GPs and all that and [we’re really thankful for that].
But when it’s life or death, that’s not good enough. It’s just not good enough.
I see my clients [in my work as an occupational therapist] go for assessments and treatments that I know my friends don’t go to because they’re not a WorkSafe or ICBC client. So I already know that there’s other stuff out there and it’s the same for cancer treatment – or any kind of treatment, really. Whatever the diagnosis would’ve been...if it’s a life or death thing? Yeah, I had no hesitation.

What advice would you give someone recently diagnosed with cancer? What advice do you wish you’d been given when you first received your diagnosis?
I think my advice to them would be to look outside the medical system.
Because even Inspire Health – and although there are lots of things wrong with it – it was the first thing that I found that was outside the medical system that supported me in areas that the cancer clinic didn’t. When I found Inspire health, it was like, here’s something else that I can do, that can empower me.
And to anyone who asks us what to do, we [tell them about] CTOAM. And we’ve now done that with about 4 or 5 different people who’ve come to us.
What I say to them is, "you need to be in charge of [your cancer care]. You need to do more than what the oncologist is telling you and sending you to treatments – you need to know more."
It’s too bad that the medical system can’t tell their patients about these outside resources that cost money. And just give people the choice, whether they [end up doing it or not].
I think it’s about that power piece and empowering yourself, however you do that. CTOAM worked for us, so that’s why it’s my recommendation. But if you find other ways, then go for it.
You need to educate yourself.
Like, we were in the North Van cancer clinic getting treatment one time. So, first, they walk around with candy (sugar) to offer you – and it’s like, "okay...just feed the tumours while you’re trying to kill the tumours...?!" [Sugar is known to exacerbate cancer.]
And then, the dietician happened to be beside us talking to someone else and [we overheard their conversation]. It was a gentleman with cancer. And the dietician says to him, "so, your main goal on chemo is to not lose weight. You can eat McDonald’s, you can eat whatever you want, just do not lose weight on chemo."
And we were like, are you kidding me? Like, seriously. This is the dietician’s advice in the cancer clinic in North Van. I just couldn’t believe. [Fatty foods and processed foods are also known to exacerbate cancer.]
You need to be educated. You need to know.
It’s also really important to focus on the positive stuff and make an effort to go to a place of hope and happiness as much as possible.
Because if you have that in the background – if you constantly have that hope in your mind because it’s scientifically there – I think that really helped my brain just stay honestly positive.
You know, it’s the same as anxiety. It’s like, my brain is telling me not to be anxious, but I’m still anxious.
So this [CTOAM and the evidence-based treatment] was a real hope that honestly helped keep my anxiety and those sorts of things down anyways, compared to if there was no hope.
The overriding hope came from having this science foundation, which meant that I knew I was getting the best treatment I could be.
So that’s what CTOAM provides – that anchor of science and treatment. Knowing that’s being looked after and that that’s being fought for was huge. And then it was like, well now let’s bring everything else in [meditation, yoga, relationships, etc.] and let’s just do whatever we can.
–––
Thank you so much to Joan for sharing her experience with us. Joan has now been cancer free for three years.
If you’ve received a cancer diagnosis, please email or call us today to learn how to access the most advanced tests and treatments for your form of cancer. Register for a Precision Second Opinion to discover how we can help you to reduce stress and dramatically increase treatment success.
CTOAM | Precision Oncology Consultants
Shaping the advancement of cancer care, one person at a time