
Breast Cancer Success Story: Lisa (age 54)
Get a Precision Second Opinion now!
Patient Presentation: ER Positive Breast Cancer
Seven years ago, 54-year-old Lisa found a lump in her breast and she was diagnosed with estrogen (ER) positive breast cancer. She had it removed six weeks later, but the cancer had spread to her skull and spine. Her local cancer agency warned her of the cancer’s aggressive nature; they didn’t know how to cure it. As more tumours cropped up, Lisa had additional surgery and four rounds of radiation treatment.
This approach helped, until it didn’t. When Lisa started feeling worse, her oncologist informed her that they had no more options for her aside from standard chemotherapy. This concerned Lisa because of the very low response rates and serious side effects.
Lisa wasn’t ready to accept this and so she reached out to CTOAM.

Breast Cancer Success Story
How CTOAM Helped Lisa
1. Introduced Advanced Diagnostics
We obtained a sample of Lisa’s tumour tissue and sent it for tumour DNA sequencing. We looked for cancer causing mutations in the DNA of over 340 genes involved in breast cancers.
Secondly, we asked Lisa to contact an independent community oncologist near her home town that we had experience working with, and suggested that she get a PET/CT to establish the exact state of her disease.
Understanding Cancer Diagnostics
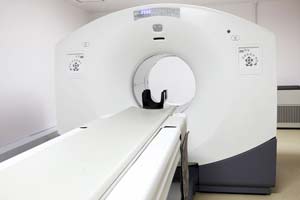
What is a PET/CT Scan?
PET/CT, unlike other forms of medical imaging, is able to identify active tumours at a very small size, based on the biological activity of the tumour.
While most forms of imaging look at the density of the tumour and compare it to the surrounding tissues, PET/CT uses a harmless radioactive isotope that is bound to a sugar molecule.
Since tumour cells are constantly growing and therefore highly metabolic, they drink up more of the sugar-isotope solution than the surrounding tissues, and any tumour will glow like a Christmas tree light.
Since only live tumours will drink the sugar-isotope solution, PET/CT can tell if a tumour is alive or if it has been affected (killed) by a specific treatment. No other form of imaging can reveal this essential information!
Furthermore, since the amount of the sugar-isotope solution a specific tumour drinks depends on how fast it is growing, a PET/CT can determine how aggressive a specific tumour is compared with other tumours in the body.
This can allow doctors to focus surgery and treatments on the tumours that are most likely to metastasize.
Luckily, after some urging, Lisa’s public system oncologist arranged for a free PET/CT for her.

2. Conducted Patient Specific Research
From our previous experience with this type of cancer, we knew that there was extensive data showing that a combination of two new drugs, called palbociclib and fulvestrant, would provide significant increases in disease free and overall survival rates for postmenopausal women with metastatic ER positive breast cancer that had failed all other options.
We also had clinical trial data showing that a specific type of drug used to prevent bone loss, called zometa, also had cancer fighting properties and provided a survival benefit for post-menopausal women with ER positive breast cancers.
The drug that she was currently taking for bone loss, called pamidronate, had no such benefits.
Next, we asked Lisa to request that her public system oncologist provide her these drugs.
Understanding Breast Cancer Treatment
What is Palbociclib?
Palbociclib is a CDK4/6 (cyclin-dependent kinase) inhibitor. CDK’s are proteins that allow a cell to go to the next stage of the cell cycle while they are reproducing. In many cancers, CDK’s are over-activated and this allows cells to move quickly through the reproduction cycle without any regulation.
In women with advanced estrogen positive breast cancer, the addition of palbociclib to the anti-estrogen drug letrozole resulted in an increase of the median progression-free survival (PFS) from 10.2 months to 20.2 months.
What is Fulvestrant?
Women with estrogen positive breast cancer typically take drugs to inhibit the production of estrogen, which drives the progression of this type of cancer. The most common drugs are steroidal inhibitors, such as exemestane, and nonsteroidal inhibitors, such as anastrozole and letrozole. These drugs work by inhibiting a key component (aromatase enzyme) of the estrogen synthesis process.
Unfortunately, there are many side effects to inhibiting estrogen production and, eventually, the cancers become estrogen independent and develop resistance to these drugs.
The reason for this is as follows. Firstly, there are two estrogen receptors that estrogen binds to, and they are called estrogen receptor alpha (ERa) and estrogen receptor beta (ERb).
When estrogen binds ERa, it causes the breast cells to proliferate and grow fast. However, when estrogen binds to ERb, it causes the cells to stop growing.
As you can imagine, the primary driver in breast cancer is the ERa, and when cancer becomes resistant to these drugs (estrogen independent), it is due to the ERa gaining the ability to self-initiate without the need for estrogen binding.
Fulvestrant works by binding to and degrading the ERa, and therefore allows for a much more effective reduction in ERa signalling. Furthermore, it can be combined with an aromatase inhibitor for a much greater overall reduction.
Interestingly enough, Lisa’s public system oncologist agreed that the ideal drug combination would be for her to go on palbociclib and fulvestrant.
Furthermore, her oncologist told her she could provide her with a clinical trial for fulvestrant, but not palbociclib.
In fact, her public system oncologist claimed she had even gone as far as to call the drug maker but was told that Lisa could not receive the drug for free because she was at an advanced stage of disease.
Regardless, Lisa was thrilled that her public system oncologist had agreed with our conclusions for interim treatment.

4. Clinical Trial Support and Advocacy
Based on our research and experience with these drugs, we knew that the drug makers of these drugs often had compassionate access programs and that, although some of these drugs may be available individually via clinical trials, we could more than likely get most of them provided for free by the manufacturers.
We then had Lisa contact a community based oncologist that we worked with, and together we were able to provide her with access to palbociclib, fulvestrant and letrozole.
Lisa did need to pay for the Zometa out of pocket, which typically costs less than $800 per year.
5. Genetic Testing During Treatment
During the course of her treatment, Lisa’s DNA sequencing results came in.
As we suspected, the tumour DNA sequencing confirmed that the quadruple drug regimen we had originally suggested would provide significant benefits for Lisa.
Furthermore, Lisa had a BRCA2 mutation that had previously been missed by her public oncologist and BCCA’s inherited genetic testing program. We had suspected that due to her young age, Lisa was more than likely harbouring an inherited genetic mutation as it is unlikely for a person with a healthy lifestyle under the age of 50 to get cancer.
While this mutation was rare, we uncovered peer review studies showing it was indeed a causative mutation that was responsible for her disease, and more than likely inherited.

Will Radiation Work for Breast Cancer?
How Lisa’s Genetics Impacted her Treatment
We were also able to confirm for Lisa that due to her BRCA2 mutation, any radiation treatments would have significant benefits for her compared with other cancer patients that did not have this mutation.
Furthermore, this mutation opened the door for a variety of potential targeted treatments including a new class of drugs called PARP inhibitors, and PD-1R/L checkpoint inhibitors, which are a new type of immunotherapy that has minimal side effects.
Understanding Breast Cancer Treatment
What are PARP Inhibitors?
PARP inhibitors work by targeting a signalling mechanism involved in DNA repair. Since Lisa’s faulty BRCA2 gene is also involved in DNA repair, using a PARP inhibitor would result in her tumour cells being unable to repair DNA damaged by standard radiation (RT) and chemotherapy.
In other words, the addition of a PARP inhibitor would provide significant benefits to standard chemotherapy and radiation. This approach is referred to as ‘synthetic lethality’.
What are PD-1R/L checkpoint inhibitors?
The PD-1 ligand is a protein that every cell in the body is required to have on its outside surface. It acts much like a security guard in that it tells the immune system that the cell is a normal body cell, so when the PD-1 ligand binds with the PD-1 receptors on the immune cells, it disables them.
In these cases, the tumours have a blanket of PD-1 ligand surrounding them, allowing them to turn off the immune response.
This is one of three known mechanisms that tumours use to avoid detection by the immune system. The other two are known as the CTLA4 and the IDO axis.
How Mutations Influence Treatment
So why is this important? Because Lisa’s tumours have a high amount of mutations, they are able to initiate a massive response by the immune system in order to hijack its growth factors and resources. They then use mechanisms such as over expression of PD-1, CTLA4, and IDO to prevent getting attacked by these same immune cells.
In a recent study of women with advanced ER positive breast cancer, combining a PD-1 inhibitor with standard chemotherapy resulted in a 34% response rate compared with only 13% for chemotherapy alone. More importantly, the responses from PD-1 inhibitors were very durable and had minimal side effects compared with standard chemotherapy and radiation.
6. Patient Outcome
The combination of palbociclib, fulvestrant, letrozole and zometa is working very well for Lisa and has resulted in a significant reduction in her disease. In fact, a recent PET-CT showed a reduction in many of her tumours, and she reports that it has been many years since she has felt so well. Additionally, Lisa was able to get some of the drugs covered through compassionate access, with the help of our cancer advocacy services. So, she got the treatment she needed with much less stress and without the harsh side effects and limited benefits that chemotherapy would have provided her. Furthermore, when these drugs stop working, she has a variety of other targeted therapies that have the potential of providing her with more time, without the damaging side effects of standard chemotherapy.7. Conclusions
As you can see, CTOAM’s advanced diagnostics, records review, and consultations can result in significant benefits to a patient’s outcome. Having access to a team of precision oncology specialists, doctors, and patient advocates can make all the difference in the outcome of your disease.
If you or a loved one has cancer, contact us today so we can do a brief review of your medical records. CTOAM’s cancer research and patient advocacy experts will ensure that you have access to the most advanced tests and treatments available for your unique form of cancer – for as to home, as possible.
Get a Precision Second Opinion now!
Changing the face of cancer care, one person at a time.