
Precision Oncology Success Story: Sherri (age 56)
Get a Precision Second Opinion now!
Sherri’s Story Breaks Our Heart! We Want to Help You Avoid the Same Fate
Read Sherri’s story below to see why it’s critical to get Precision Oncology help from experts like CTOAM as soon as possible. Simply put, the earlier you contact us, the better chance you have of getting the right treatment.

Patient Presentation:
Metastatic Stage IV Non-small Cell Lung Cancer (NSCLC)
Sherri was a 56-year-old woman living in Alberta, Canada, who was first diagnosed with metastatic stage IV NSCLC in February 2018. Sherri’s public oncologist decided to do a small tumor DNA sequencing test to determine if targeted therapies would be an option for her.
Luckily, this test showed that Sherri was one of the few NSCLC patients whose cancer was driven by an EGFR L858R mutation. While EGFR mutations only occur in a small number of NSCLC cases, there are a variety of EGFR targeted drugs that can greatly increase the survival rates of these patients – without the harsh, debilitating side effects of standard chemotherapy.
In March 2018, Sherri’s oncologist prescribed the well-known EGFR targeted drug, Afatinib, which she tolerated very well. Importantly, a CT scan in late June showed that her main tumor had decreased from 3.2 cm to 2.1 cm. It also showed that other tumors had disappeared, and some lymph node tumors had also decreased in size. Both Sherri and her oncologist were happy with this outcome.
However in October 2018, Sherri experienced increased coughing episodes and returned to her oncologist. Her oncologist informed her that there were only subtle changes in a recent CT scan from September – and that these changes did not warrant a change in her current treatment protocol. He also said it wasn’t necessary to do any further genetic testing (to look for secondary mutations that could have resulted in resistance to her current therapy).
Her oncologist assured Sherri that her current treatment was working as it was supposed to.
Sherri was not willing to accept this outcome, so she reached out to CTOAM for a Second Opinion. We helped Sherri access advanced diagnostic and treatment technologies that were otherwise not yet available to her through the public medical system.
How CTOAM Helped Sherri
1. Performed an Extensive Medical Records Review
First, we examined Sherri’s medical records. Sherri’s oncologist had prescribed a well known targeted drug,
Afatinib. This is a second generation EGFR inhibitor that can provide great benefits to patients. However,
most patients eventually become resistant to this drug due to new emerging mutations in the EGFR gene (like
the EGFR T790M, as well as mutations in another gene called MET).
Importantly, there are newer, more advanced targeted therapies for both of these mutations if a patient’s initial treatments stop working.
In January 19, 2018, Health Canada approved the use of Tagrisso. Tagrisso is a third generation EGFR inhibitor with prominent activity against both the standard activating EGFR mutations (EGFR L858R), as well as the treatment resistant EGFR T790M.

Tagrisso has been shown to greatly extend the life of patients with EGFR mutations compared to first and second generation drugs such as Afatinib. And, significantly, patients do not relapse if they develop the emerging EGFR T790M mutation. Simply put, this drug is vastly superior to all other EGFR inhibitors and has far fewer side effects.
We were shocked to see that even with the approval of this drug in January 2018, Sherri’s oncologist has prescribed an inferior drug. We immediately sent Sherri’s oncologist the application forms for this drug. Unfortunately, because Tagrisso had only been approved as a first line treatment, and Sherri had already been prescribed Afatinib, she would now need to pay out of pocket for the Tagrisso.
We also noticed that Sherri’s oncologist had ordered a PD-1 test. The results had showed that Sherri had a very high level, which indicated that she would be an excellent candidate for Immune Checkpoint Inhibitors. In April 2018, Health Canada approved the PD-1L inhibitor, Atezolizumab, as a mono-therapy for the treatment of adult patients with locally advanced or metastatic NSCLC with progression on or after platinum-based chemotherapy. Additionally, this drug has also been approved for patients that have progressed after taking EGFR inhibitors like Afatinib.
Understanding NSCLC
About Immune Checkpoint Inhibitors
In short, programmed death one (PD-1L) is a protein that allows the immune system to distinguish between normal body cells and pathogens/cancer cells. However, some cancers (like Sherri’s) produce a bubble of PD-1L around them to protect themselves from the immune system. When the immune cells see this PD-1L bubble, they’re tricked into thinking the tumors are normal body cells and they leave them alone.
PD-1L inhibitors act like a sponge to remove this protective bubble around the tumors, resulting in a rapid response from the immune system against the tumors. When these drugs work, they lead to durable long-term remissions and, in some cases, cures. CTOAM was one of the first in Canada to use PD-1 inhibitors with a cancer patient, nearly five years ago. At the time, that patients had been given just months to live – and now, thanks to immunotherapy and CTOAM, she’s been cancer free for almost five years!
These drugs result in excellent survival rates in the patients with NSCLC that have high PD-1L expression, such as Sherri.
However, Sherri’s oncologist would not prescribe this drug to her unless she was no longer responding to Afatinib. And, in his opinion, she was still responding to the Afatinib
So, our immediate goal was to confirm whether or not Sherri was still responding to Afatinib.
Our second goal was to determine if Sherri was developing treatment resistant mutations, such as the EGFR T790M.
2. Introduced Advanced
Diagnostics
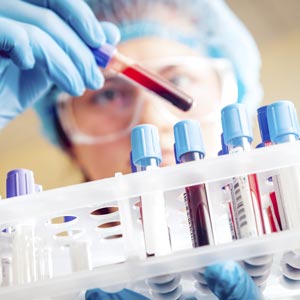
Since we knew Sherri had an EGFR L858R mutation, we used an advanced form of Liquid Biopsy known as,
Exosome-Based Liquid Biopsies. Recent discoveries have shown that cancer cells release cancer-causing DNA
mutations (like the EGFR L858R) in membrane bound packages called exosomes. These exosomes travel throughout
the body via blood and convert normal cells into cancer cells.
While other Liquid Biopsies measure the amount of a specific mutation in the blood, they do not differentiate from where the mutation comes from. In other words, while Sherri’s blood may contain a high level of her EGFR mutation, these tests would not be able to tell if the mutation is from dead tumor cells that have released their DNA into the blood due to effective treatment, live tumor cells that are travelling in the blood that may spread, or from exosomes.
Learn More About Exosome-Based Liquid Biopsies
By focusing on exosome-based tumor DNA, this revolutionary Liquid Biopsy test allows us to identify the ratio of Sherri’s cancer-causing EGFR mutation – and compare it to the normal or Wild Type version of the gene, and quantify it in a relative percentage. In other words, we can see if the mutation fraction that is directly associated with metastasis is increasing or decreasing.
The result is that exosome-based Liquid Biopsies allow us to identify a metastatic process in the very early stages, well before it would show up on even the most advanced imaging tests (like PET-CT).
Further, since new emerging mutations in the EGFR gene often occur after treatment with Afatinib, we also tested Sherri’s blood for the emerging EGFR T790M mutation, which has been shown to create resistance to EGFR inhibitors such as Afatinib. If we found this mutation, we would have a better a better chance of getting Tagrisso approved for Sherri.
Unfortunately, the results of this Liquid Biopsy showed an elevated level (11.28%) of her EGFR L858R mutation. This revealed that, while her September CT scan had showed only subtle changes, in reality her disease was in full progression and she was no longer responding to Afatinib – contrary to what her oncologist had, incorrectly, assumed.
More importantly, Sherri’s Liquid Biopsy was negative for the emerging treatment resistant EGFR T790M mutation. This indicated that a different mutation, such as MET, was likely the cause of her cancer’s progression.
With this in mind, we immediately arranged for Sherri to get a PET-CT to identify the exact progression of her disease and to prove to her doctors that she was no longer responding to Afatinib.
In late October, we arranged for a private PET/CT from Premier Diagnostic Center. This local company is our first choice for PET/CT scans because it offers:- Very fast results
- Low cost compared to other clinics
- Excellent radiologists
Understanding Cancer Diagnostics
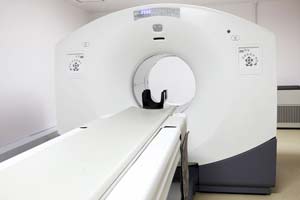
What is a PET/CT Scan?
PET/CT, unlike other forms of medical imaging, is able to identify active tumours at a very small size, based on the biological activity of the tumour.
While most forms of imaging look at the density of the tumour and compare it to the surrounding tissues, PET/CT uses a harmless radioactive isotope that is bound to a sugar molecule.
Since tumour cells are constantly growing and therefore highly metabolic, they drink up more of the sugar-isotope solution than the surrounding tissues, and any tumour will glow like a Christmas tree light.
Since only live tumours will drink the sugar-isotope solution, PET/CT can tell if a tumour is alive or if it has been affected (killed) by a specific treatment. No other form of imaging can reveal this essential information!
Furthermore, since the amount of the sugar-isotope solution a specific tumour drinks depends on how fast it is growing, a PET/CT can determine how aggressive a specific tumour is compared with other tumours in the body.
This can allow doctors to focus surgery and treatments on the tumours that are most likely to metastasize.
Unfortunately, as expected, the PET/CT confirmed that Sherri’s disease had progressed significantly. Not only did she have new tumors in her liver and bones, but there were numerous PET-CT features of an extremely aggressive process, with extensive progression in the interval of her last scan and new pleural effusions.
We shared these results (from the PET-CT, along with the results from our exosome-based Liquid Biopsy test) with Sherri’s oncologist – who scheduled her immediately for an appointment.
3. Conducted Patient
Specific Research
In order to determine if Sherri’s tumours contained any further targetable mutations, we obtained a sample of
her tumor and sent it for a more extensive tumour DNA sequencing test.
Tumor DNA sequencing looks at a variety of targetable genetic mutations in the DNA of tumour cells.
Unfortunately, the tumour DNA sample submitted was not adequate for sequencing.
4. Clinical Trial Support and Advocacy
With these findings, we wrote a white paper for Sherri’s oncologist with suggestions for further treatment.
In our report, we provided Sherri’s oncologist with new data that showed that Tagrisso, while currently only approved for first line treatment, also showed significant benefits and survival rates in NSCLC patients as a second and third treatment – even if the patient does not have the EGFR T790M mutation.
We also provided new data regarding a drug, Zometa, which is normally used for bone loss, and might provide significant benefits to Sherri:
The drug, Zometa, is normally prescribed for breast cancer patients to prevent bone loss. However, a previous study of 311 NSCLC patients with bone metastases found that this drug not only increased the survival in advanced patients from 275 days to 385 days, but also reduced the incidence of malignant pleural effusion in these patients.
We also shared our data that Sherri’s progression was not due to the emerging EGFR T790M mutation, but was more than likely due to an emerging MET mutation.
Sherri’s oncologist was very receptive to our information and immediately started the process of enrolling Sherri in a clinical trial for a new MET targeted drug.
We also urged Sherri to get a drain port put in to reduce the pleural effusion, since it was Flu season and Sherri had not had a Flu vaccine. Unfortunately, Sherri was told by her emergency doctor that her effusion was not bad enough to require a port at that time.
Sadly, Sherri contracted a bad infection soon after and died in mid-December 2018. We believe her pleural effusion played a role in this infection.
We also believe if Sherri had contacted us earlier, the outcome would have been very different – and that, based on existing peer reviewed science, Sherri would have lived many years longer.

Conclusions
As you can see, CTOAM’s advanced diagnostics, records review, and consultations can result in significant benefits to a patient’s outcome. Having access to a team of precision oncology specialists, doctors, and patient advocates will make all the difference in the outcome of your disease – especially if you contact us early on.
If you or a loved one has cancer, reach out today so we can do a brief review of your medical records. The CTOAM team will ensure that you have access to the most advanced tests and treatments available for your unique form of cancer...as close to home as possible.
Get a Precision Second Opinion now!
Changing the face of cancer care, one person at a time.