
Carcinoma Success Story: Mark (age 53)
Get a Precision Second Opinion now!

Patient Presentation: Stage IV Esophageal Squamous-Cell Carcinoma
Mark is a 53-year-old man from British Columbia, Canada, recently diagnosed with stage IV esophageal squamous-cell carcinoma. A CT scan provided to him by his public system oncologist found a significant mass in his esophageal-stomach junction, with possible metastasis to the liver.
Mark was a heavy smoker, had a very poor diet, and had been unable to keep food down for some time. In fact, he had lost so much weight that he was unable to do even the most basic physical activities.
Although standard chemotherapy would have been able to provide him with a year or two of survival, Mark’s doctors told him that since there was the potential of liver metastasis, treatment with standard chemotherapy was not an option for him.
Mark’s oncologists suggested that he get low dose palliative radiation therapy and told him to get his affairs in order.
Mark was not willing to accept this outcome, so he reached out to us for a second opinion. We helped him access advanced diagnostic and treatment technologies not yet available through the public medical system.
Carcinoma Success Story
How CTOAM Helped Mark
1. Introduced Advanced Diagnostics
Since the potential of chemotherapy would be based on whether or not Mark had metastasis, we arranged for a private PET/CT from Premier Diagnostic Center. This local company is our first choice for PET/CT scans because it offers:
- Very fast results
- Low cost compared to other clinics
- Excellent radiologists
The radiologists at Premier Diagnostic Center report the SUVs (Serum Uptake Value) of every tumour – unlike many other clinics we have dealt with. Please note that CTOAM has no financial affiliation with Premier Diagnostic Center: our only goal in recommending them is to offer patients the most benefit.
Understanding Cancer Diagnostics
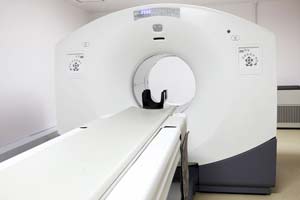
What is a PET/CT Scan?
PET/CT, unlike other forms of medical imaging, is able to identify active tumours at a very small size, based on the biological activity of the tumour.
While most forms of imaging look at the density of the tumour and compare it to the surrounding tissues, PET/CT uses a harmless radioactive isotope that is bound to a sugar molecule.
Since tumour cells are constantly growing and therefore highly metabolic, they drink up more of the sugar-isotope solution than the surrounding tissues, and any tumour will glow like a Christmas tree light.
Since only live tumours will drink the sugar-isotope solution, PET/CT can tell if a tumour is alive or if it has been affected (killed) by a specific treatment. No other form of imaging can reveal this essential information!
Furthermore, since the amount of the sugar-isotope solution a specific tumour drinks depends on how fast it is growing, a PET/CT can determine how aggressive a specific tumour is compared with other tumours in the body.
This can allow doctors to focus surgery and treatments on the tumours that are most likely to metastasize.
Unfortunately the PET/CT showed that Mark had a massive 6.4cm tumour in his esophageal-stomach junction that had an SUV = 8.5, and additional metastasis in his liver.
Secondly, we had Mark contact a local oncologist who was prepared to offer Mark off-label targeted drugs should the scientific evidence indicate a benefit.
Understanding Cancer Treatment
What are Targeted Therapies?
Standard chemotherapy drugs work by inhibiting any rapidly reproducing cells in the body. Typically, these drugs interfere with a cell’s ability to replicate; however, they are not specific to cancer cells and will kill any cell that happens to be reproducing during treatment.
This unfortunately results in many harsh and permanent side effects.
Furthermore, standard chemotherapy drugs do not typically target the actual cancer-causing stem cells that create the bulk of the tumours, as these unique cells are resistant to standard chemotherapy.
Targeted drugs work by targeting genetic or molecular alterations that are ONLY found in your tumour cells, and do not typically affect your normal healthy cells.
2. Conducted Patient Specific Research
In order to determine if Mark’s tumours contained any targetable mutations, we obtained a sample of his tumours and conducted an extensive panel of tests, including tumour DNA sequencing and HER2 testing.
Tumour DNA sequencing looks at a variety of targetable genetic mutations in the DNA of tumour cells, and HER2 is a targetable molecular feature common to breast cancers that has recently been found in certain stomach cancers. Patients that have high HER2 respond well to the drug Herceptin.
Unfortunately, the tumour DNA sequencing did not reveal any known targetable alterations, and all of his mutations were unknown and unique to him.
While this is not a common occurrence for us, we can still use the unknown genetic mutations to perform an analysis using computer-based modelling.
Our computer based modelling indicated that Mark’s tumour would more than likely respond to a certain class of drugs called programmed death one (PD-1) immune checkpoint inhibitors.
Understanding Cancer Treatment
What are PD-1 and checkpoint inhibitors?
The PD-1 protein is found on the surface of all body cells and tells our immune system that the cell is part of our body and NOT a foreign invader. Some tumours escape being attacked by our immune system by producing massive amounts of PD-1 protein, and in doing so, form protective blankets around themselves.
PD-1 inhibitors work by acting like sponges and soaking up any excessive PD-1. This allows the immune system to recognize the tumours, often resulting in massive and durable responses against the cancers cells.
It is thought that once the immune system has been disabled by the PD-1 blanket that surround a particular tumour, then it does not return again to the same site, as it views any further tumour-like activity as a false alarm. In other words, all tumours will at one time express PD-1, but will do so at different times during the course of the disease.
Additionally, we found that diet and exercise had a strong role in reducing the growth potential of this specific metabolic based tumour, so we created a tumour-fighting diet and exercise plan for Mark, which he followed faithfully.

Since our computer modelling indicated that Mark would potentially respond to PD-1 inhibitors, we performed a PD-1 ctRNA liquid biopsy blood test. This test measures the amount of PD-1 protein. The higher the level, the better the response to these drugs is.
While most commercial PD-1 tests examine the amount of PD-1 from a single biopsy sample, ctRNA measures the amount of PD-1 body-wide. This is important because, as previously noted, not all tumours in the body will produce the immune disabling PD-1 blanket at the same time.
Since the liquid biopsy detects circulating PD-1 protein (ctRNA) body-wide, it provides us with a rough idea of the total amount of PD-1 ligand produced by all of Mark’s cancer cells.
The liquid biopsy test showed us that Mark’s PD-1 protein levels were over 10.4 times higher than the normal body levels, indicating the potential for a significant response from PD-1 inhibitors.
We immediately shared this information with Mark’s new oncologist, and he arranged for immediate infusions of the PD-1 inhibitor drug pembrolizumab.
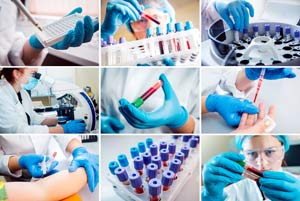
4. Testing During Treatment
After a few treatments with pembrolizumab, Mark reported feeling much better. His body weight started to improve as his tumour markers started to drop.
Importantly, a PET/CT showed a decrease in the SUV of his stomach tumour, going from 8.55 prior to treatment, down to SUV = 4.
This reduction in tumour activity allowed Mark to have his feeding tube replaced with a stent. Remarkably, when the surgeon put in his stent, he could find no evidence of the massive 6.5 cm tumour that was previously blocking his esophagus.
5. Clinical Trial Support and Advocacy
After reviewing the latest gastrointestinal conferences, we gathered new research showing that when patients with esophagus cancers were given a drug called a MEK inhibitor (trametinib), these patients responded much better to PD-1 inhibitors.
In fact, our initial computer modelling analysis also indicated that a MEK inhibitor could potentially help Mark. It is thought that in certain genetic backgrounds, the MEK inhibitor stimulates an immune response.
Pembrolizumab and Trametinib
We presented this new plan to Mark and his treatment team. Should his cancer progress, this combination will be considered.
6. Patient Outcome
Recently, Mark reported that he has gained another 24 pounds since his last infusion.
Although his recent PET/CT did show an increase in liver metastasis, we believe this is a false positive result, which is common with immune therapies. (Immune therapies stimulate the immune cells to enter the tumours, making them appear much larger initially when imaged.)
However, this initial false positive response is typically followed by a reduction in SUV values, indicating a less active tumour.
Importantly, when patients respond to PD-1 inhibitors, the responses are very durable. We have seen many cases where after only two to three treatments, the tumours never came back. We do hope this is the case with Mark, and will be updating this report in the near future.

Conclusions
As you can see, CTOAM’s advanced diagnostics, records review and consultations can result in significant benefits to a patient’s outcome. Having access to a team of precision oncology specialists, doctors, and patient advocates can make all the difference in the outcome of your disease.
If you or a loved one has cancer, contact us today so we can do a brief review of your medical records. CTOAM’s cancer research and patient advocacy experts will ensure that you have access to the most advanced tests and treatments available for your unique form of cancer – as close to home as possible.
Get a Precision Second Opinion now!
Changing the face of cancer care, one person at a time.